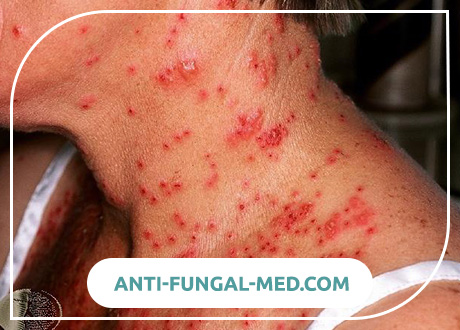
What is Herpetic Eczema?
Herpetic eczema (old names: varioliform pustus Kaposi-Juliusberg, herpetic eczema Kaposi, Kaposi syndrome, acute openenoblute pustus Juliusberg) – is a disseminated herpes virus infection, complicating the course of chronic dermatoses with erosive populations, shepatitis, which is difficult, with age, age, age, venous tumors, chromosomal vaginosis, nodules, chromic aneurysmus ecstatic , and developing on the background of immunity disorders.
Hungarian scientist Kaposi M. in 1887 described the characteristic changes in the skin and associated them with a general violation of the patient’s condition. In 1883, Kaposi called this disease a herpetiform eczema – “eczema herpetiforme”. In 1898, Jliusberg S. described this dermatosis as “pustulosis acuta varioliformis” and suggested its viral etiology. In the concept of “acute varioliform pustus,” he included both rashes observed in herpes eczema and rashes that occur in response to the introduction of the vaccine strain of variola virus or the patient’s contact with chronic dermatosis with children who received the smallpox vaccine. This combination of two diseases similar in clinical picture for a long time hampered the epidemiological investigation. Currently, such errors are excluded, since due to the elimination of the incidence of smallpox and the cessation of smallpox inoculations, the occurrence of vaccines is impossible.
Despite the fact that in 1912 the herpes simplex virus (HSV) was isolated by Gruter W., and in 1941 Esser M. and Seidenberg S. and Ruchman A. and Welsh A. in 1947 proved that the causative agent for hepatic eczema is HSV, in the domestic dermatology up to the 1950s and 1960s, the concepts of vaccines and herpes eczema were not divided. In our country, the etiological role of HSV in the development of herpetic eczema was confirmed by ELL Kiefer (1958) and A.A. Vitko (1970).
A great contribution to the study of herpetic eczema was made by F.A. Zverkov, S.Ya.Golosovker, who in 1955 for the first time in Russia described 10 patients with this dermatosis. During all subsequent years, the study of the features of epidemiology, clinic, course of the disease and improvement of therapy continued.
Currently, the numerous old names of this dermatosis, which were previously used by dermatologists, have been replaced by the term herpetic eczema, which, in our opinion, most clearly reflects the nature of this dermatosis and is convenient for diagnosis.
Causes of Herpetic Eczema
Today, herpetic eczema is commonly thought of as a form of herpes simplex (Herpes simplex), or simple bubble lichen. The causative agent of herpes infection is a DNA-containing HSV. Most researchers divide HSV into two types: HSV-1 and HSV-2 (Herpesvirus hominis typus 1, typus 2). Overwhelmingly, HES is caused by HSV-1.
It is noted that herpetic eczema often develops in children who have atopic dermatitis occurred earlier in the 2nd month of life. Most of the children suffering from herpetic eczema from an early age were breastfed.
The incidence of herpetic eczema is higher in children aged 6 months. up to 2 years, in adolescents and adults, herpes eczema is rare. The occurrence of this complication in early childhood is due to a sharp drop in intrauterine transmitted antibodies to HSV by 6 months. life and the appearance of its own antibodies to the herpes virus only to 2-3 years. According to A.A. Vitko, who studied antibodies to HSV in young children, the dynamics of change in the amount of antibodies is as follows: in children aged 4 days to 5 months. in 94% of cases, antibodies to HSV were detected, in children from 6 to 12 months. – in 20%, and in the age from 1 year to 2 years the number rises to 60%, since the child already has its own antibodies. This explains the peak in the incidence of herpetic eczema attributable to 7–12 months of a child’s life.
The risk group consists of children with ARVI and receiving topical therapy with glucocorticosteroids, as well as children and adults on immunosuppressive therapy for hemato-oncology and other somatic pathology.
Pathogenesis during Herpetic Eczema
The source of infection of children is a person with herpes simplex, most often it is the closest relative (mother, father, etc.). Often, when examining relatives, it is possible to detect residual effects of herpes simplex, localized mainly on the lips, nose wings, conjunctiva of the eyes, hands. Ways of transmission of the virus are varied. The main should be considered airborne and direct contact transmission paths. Infection occurs when it comes into contact with the affected skin, oral mucosa, and patient’s saliva. HSV is inactivated at room temperature for 10 hours, so infection by airborne droplets as well as through household items is possible. In patients with herpes simplex, the virus is secreted from various secrets depending on the location of the lesions (saliva, tears, vesicle contents).
Symptoms of Herpes Eczema
The incubation period is usually 2-7 days, sometimes it can be extended to 10 days. A seasonal increase in the incidence of herpetic eczema is observed in the second half of autumn, in winter, and also in early spring.
Herpetic eczema complicates the course of chronic dermatoses, in which there are erosive and ulcerative lesions of the skin. In 90-95% of cases of herpetic eczema develops in patients with atopic dermatitis. 5-10% is due to other chronic dermatosis. The literature describes cases of herpetic eczema on the background of seborrheic dermatitis, chronic eczema, benign family pemphigus Guzhero – Haley – Hayley, Darya disease, with thermal burns, acne, fungal mycosis, vulgar pemphigus.
In most cases, characterized by acute onset. In some cases, the acute period is preceded by a prodromal period, during which drowsiness, lethargy, indifference of the child is observed.
The duration of the prodromal period can be 1-3 days and ends with a sharp deterioration in the general condition of the child and the rise in body temperature to 39-40 C. Breathing and pulse rate. Thus, in severe herpetic eczema, severe toxicosis is manifested, manifested by severe shortness of breath, tachycardia, muffled heart sounds, and convulsions, anorexia, and other neurological symptoms can join. In a number of patients, the disease can occur in a milder form, characterized by a rise in body temperature of up to 38 ° C, a relatively satisfactory general condition of the patients without visible signs of toxicosis. The febrile period lasts on average 6-10 days and coincides with the period of rash. It is noted that the temperature response in patients with herpetic eczema is constant with fluctuations during the day within one degree and is not easily affected by antipyretic drugs.
The most frequent localization of lesions: the skin of the face (cheeks, forehead, ear folds, ears), the scalp, neck, upper limbs (dorsum of hands, forearms), less frequently dorsum of feet, torso, buttocks. In some patients with previously severe chronic dermatoses, elements of the rash can cover the entire skin. In such cases, the rash has a generalized distribution.
The most important for the diagnosis of herpetic eczema is the presence of typical rashes on the skin (on the mucous membranes of the rash ephemeral and quickly turn into erosion), which allow to establish the correct diagnosis in a timely manner. Against the background of a sharp rise in temperature, marked edema and inflammatory erythema of the child’s face are noted. Then within 6-12 hours, papules-vesicles, vesicles with serous, serous-hemorrhagic contents, pustules appear consistently undergoing evolution. Vesicles and pustules for herpetic eczema have a typical appearance: rashes of approximately the same size (1-3 mm in diameter), dome-shaped, with umbilical depression in the center and an inflammatory roller around the periphery. Rash is abundant, characterized by herpetiform arrangement: most of the elements are grouped. It is also possible and disorderly location, often reminiscent of rash with chickenpox. On the face, pustules due to their abundance almost merge and form characteristic foci. Along the edges of foci scattered separate isolated typical pustules.
In the process of evolution, abdominal elements open up, erosion merges between them, forming huge areas devoid of epidermis, then the elements dry up, becoming covered with brownish-brown hemorrhagic crusts. Characteristic features of lesions in herpetic eczema are: increased skin vulnerability, formation of bleeding erosion, deep cracks and the layering of massive hemorrhagic crusts.
During the week, new elements may appear around the main lesion and on unaffected skin.
If the course of the disease is not complicated, hemorrhagic crusts disappear after 6-10 days. Sometimes, surface atrophy in the form of barely noticeable, rounded, slightly indented scars 3-5 mm in diameter, rarely large scars of polycyclic configuration, remain at the site of lesions.
With the appearance of vesicular-pustular eruptions typical of herpetic eczema, the clinical picture of previous atopic dermatitis usually weakens or disappears. During the period when herpetic eruptions are resolved and the patient’s body temperature is critically or lytically reduced, the clinical manifestations of atopic dermatitis or another skin process preceding herpes eczema again come to the fore.
At the same time with the rash on the skin, the mucous membranes of the oral cavity and pharynx are often involved in the pathological process – keratoconjunctivitis can develop, as well as damage to the mucous membrane of the genital organs.
In case of herpetic stomatitis, rashes are localized most often on the mucous membrane of the cheeks, gums, palate, the inner surface of the lips, on the tongue, less often on the soft and hard palate, palatine arches and tonsils. The process is limited and is a vesicular-erosive islets with remnants of exfoliated epidermis, located on the erythematous and edematous areas of the oral mucosa. Gums all over with herpetic stomatitis swollen. On the sky, merging erosive foci with scalloped contours may form. With glosses on the tongue, rare round-shaped vesicles are seen among the dense white plaque. Irritation of the mucous membrane leads to constant drooling. Due to pain, food intake is limited.
Damage to the eyes with herpetic eczema occurs in 10-15% of cases and most often occurs either in the form of conjunctivitis or in the form of keratoconjunctivitis. In case of herpetic conjunctivitis, the mucous membrane of the eyelids, the eyeball, and the edges of the eyelids are hyperemic. Characterized by moderate photophobia and lacrimation.
Herpes lesions of the genital organs are characterized by acute inflammatory manifestations. In boys, the rash is localized on the inner leaflet of the foreskin, on the head, neck and body of the penis. In girls, the labia, clitoris, and vagina are affected more often. Rash also presents with vesicles, erosions, ulcers against the background of erythema and edema, often accompanied by pain, itching. With involvement in the process of the mucous membrane of the urethra, there is pain when urinating and serous discharge from the urethra.
With extremely severe course of herpetic eczema, which occurs in 10-15% of cases (Zverkova FA – 1985, Adaskevich VP – 2001), often occurring with severe toxic-septic syndrome, mortality among patients reaches 10- 50%. Causes of death of patients are terrible complications: acute edema and stenosis of the larynx, cardiac arrhythmia, severe pneumonia, kidney damage, liver. According to FA Zverkovoy (1985), 10% of the sick children had convulsions, spontaneous spring tension, stiff neck and other meningeal symptoms due to the development of meningitis and meningoencephalitis.
In case of herpetic eczema, the development of septic complications in the form of strepto-and staphylodermia, purulent otitis, sepsis is possible. In children under one year old herpetic eczema is most severe and the development of complications in this group of patients is most likely.
In all patients, regardless of the severity of the disease, regional lymphadenitis is noted: an increase in the submandibular, cervical, occipital lymph nodes. In 60% of cases, hepatosplenomegaly is noted, in 20% – splenomegaly. In a number of patients, there is a disorder in the stool, which is expressed in its increase and dilution.
For the first time, herpetic eczema has lasted on average 10-20 days. Relapses are easier, without disturbing the general condition.
Diagnosis of Herpetic Eczema
Currently, the etiological diagnosis of herpetic eczema is established when examining patients using special molecular biological, virological, serological, cytological and immunological methods and the detection of HSV type 1 and 2. The material for cytological studies are smears imprints from scrapings of epithelium cells in the area of lesions on the skin, oral mucosa, conjunctiva, cornea, and skin.
- The most accessible for the diagnosis of HSV is a cytological examination of the contents of herpetic vesicles (sample Tsanka). At the same time, in smears prepared from fluid and cells of the bottom of the vesicle, multinucleated giant cells with intranuclear inclusions, characteristic of herpes infection, are found. However, the presence of these cells is characteristic not only of the herpes simplex virus, but also of infections caused by the varicella-zoster virus.
- The most reliable laboratory method today is a virological culture study, i.e. isolation and identification of the virus. Virus-containing material is infected with tissue culture – (diploid fibroblasts, rabbit kidney cells, human amnion cells, etc.) In infected cultures for 2-3 days, and with a large dose of the virus after 8 hours, the formation of giant multicore cells, round cells and their conglomerates, in which intranuclear inclusions are found. The method is highly specific, but extremely time consuming.
- The informative methods for diagnosing a herpes infection include isolating the virus from various cell cultures. Methods are based on the detection of viruses and viral antigens. Express methods have high specificity, but lower sensitivity compared to the virus isolation method in cell cultures. Polymerase chain reaction (PCR) is characterized by the highest sensitivity for detecting HSV DNA. PCR can be considered the most sensitive and rapid response in the laboratory diagnosis of herpesovirus infections.
- For the rapid diagnosis of HSV back in 1972, electron microscopy was proposed. Microscopic preparations are prepared from the contents of the vesicles, which are then contrasted with phosphorus-tungsten acid, and viewed in an electron microscope. To differentiate the two types of HSV from other viruses of the herpes family, they use electron microscopy and immunofluorescence methods (direct and indirect ELISA).
- Serological methods detect antibodies to HSV. The most frequently used reaction is the binding of complement (RAC) and the neutralization of the virus. As well as rtga, immunofluorescence, enzyme-linked immunosorbent assay, immune blotting. These methods have only a relative diagnostic value, since in children up to 3-6 months of life, detection of IgG antibodies may be a consequence of their passive transfer across the placenta from the mother’s body, and in older children, this may indicate a previous herpes infection. Significant is the 4-fold increase in antibody titer and the appearance of serum IgM to HSV. In CSC, cross-reactions of HSV and varicella-zoster virus are possible.
According to the results of laboratory tests, hypochromic anemia is found in peripheral blood in patients with herpetic eczema. A characteristic feature for children under the age of one year suffering from herpetic eczema is pronounced leukocytosis in peripheral blood. This fact seems to be associated with more frequent accession of a secondary infection, while older children, even in severe cases, have neutropenia or normal white blood cell counts.
For hemograms of patients with herpetic eczema, a pathognomonic sign of a decrease or complete disappearance of eosinophils in the peripheral blood at the beginning and in the height of the disease, while patients with atopic dermatitis are characterized by eosinophilia. After the disappearance of the manifestations of herpetic eczema, the number of eosinophils in the peripheral blood increases again.
Almost a third of patients have changes in the urine in the form of the appearance of protein, leukocytes 1-10 in sight.
With recurrent forms of herpetic eczema, it is advisable to include in the examination of the immune status for subsequent correction.
The diagnosis of herpetic eczema is based on anamnesis: the presence of atopic dermatitis or other dermatoses in a patient, direct contact of the child with a patient with herpes simplex 5-10 days before the onset of the disease; on the data of the clinical picture: acute onset (sharp rise in temperature to 38-39C, violation of the general condition), typical vesicular and pustular elements with umbilicate depression in the center, bleeding erosion, hemorrhagic crusts, located mainly on the face, neck, mucous membranes.
In the formulation of the final diagnosis, data from laboratory studies (positive Ttsank test, detection of serum IgM to HSV type 1 and type 2, PCR data) help.
Herpetic eczema must be differentiated from pyoderma (staphylococcal and streptococcal impetigo), herpes simplex, shingles, chicken pox.
In pyoderma, the general condition of the patient is usually not severely disturbed, there is no sharp rise in temperature, the pustular elements differ in size from each other, and have no umbilicate depression in the center. Impetiginous elements are covered mostly with loose honey crusts, whereas during herpetic eczema hemorrhagic crusts and cracks predominate.
With simple herpes, vesicular elements are not so numerous and usually localized (lips, nose wings, cheek skin, chin, genitals), vesicles and pustules often coalesce, there is no umbilicus-like impression on their tire, and in most cases the lesion affects the mucous membranes. In addition, rashes with simple herpes occur on previously unchanged skin, and in case of herpetic eczema against the background of atopic dermatitis or other dermatoses.
Shingles is characterized by a one-sided positioning of the vesicles on an erythematous base, the absence of umbilicate depression on the vesicles with serous-hemorrhagic contents, the most frequent lesion of the thoracic dermatomes or the innervation zone of the trigeminal nerve. Shingles is more common in adults, less often in children. Also characteristic of shingles in addition to skin manifestations are neurological disorders, which manifest themselves in the form of severe, unbearable pain in the area of the affected skin area, paresthesia, paresis, trophic disorders. In some cases, neurological disorders remain after the disappearance of the rash.
The clinical picture of chicken pox differs from herpetic eczema by the diffuse arrangement of spotted, papular, vesicular elements, the lack of selective localization. For chickenpox, indications of a history of contact between a child and a patient with chickenpox or shingles are characteristic.
Treatment for Herpetic Eczema
Treatment of patients with herpes eczema should be complex: taking into account the general condition of the patient, the prevalence, nature and stages of the rash, their localization, associated diseases and complications. Hospitalization of patients is required. Constant observation of the doctor in the conditions of the infection department is required. Patients with herpetic eczema must be isolated from other patients in boxed wards, because they can themselves be a source of infection for other children suffering from atopic dermatitis or other dermatoses.
Diet in patients with HES should be age appropriate. For infants recommended to continue breastfeeding. For the purpose of detoxification, frequent drinking is recommended; in case of a serious condition, transfusion therapy is indicated: intravenous infusion of 5-10% glucose solution, physiological saline with 5% ascorbic acid solution and 50-100 mg of cocarboxylase. In cases of severe intoxication, it is necessary to introduce fresh frozen plasma, 10% albumin solution 10 mg / kg baby weight. When neurological symptoms appear, patients should be consulted by a neurologist.
Etiotropic antiherpetic therapy is prescribed to patients from the first day of admission to the hospital. In pediatric practice, acyclovir is the drug of choice for treating a herpes infection. Acyclovir has become the first highly effective antiherpetic drug that blocks viral DNA synthesis and protects uninfected cells. The low toxicity of acyclovir is explained by the fact that it enters the active phase in the presence of virus-specific thymidine kinase, thus affecting only infected cells, blocking the synthesis of viral DNA and protecting uninfected cells. Acyclovir lacks immunosuppressive properties. The half-life of acyclovir from the body is about 3 hours, and 90% of the drug is excreted in the urine and unchanged. Young children suffering from HES are given acyclovir intravenously at a dose of 5 mg / kg of body weight every 8 hours for 5–8 days, and with weakened immunity, the doses are increased to 10 mg / kg of body weight per day. The appointment of acyclovir orally for adults and children over 12 years old is made at the rate of 5 mg / kg body weight every 8 hours.
From the first day, in order to increase immunity, intramuscular anti-herpes immunoglobulin is administered intramuscularly to a patient with herpetic eczema 1 dose once a day in 2-3 days for a course of 3-5 injections
At the same time, in order to reduce itching and anxiety in patients (especially during the period of subsidence of herpes), the administration of antihistamines (diphenhydramine, suprastin, tavegil, diazolin) and calcium gluconate in age dosages are indicated.
In cases of severe intoxication syndrome occurring with impaired cardiac activity, children are prescribed cardiac glycosides. It is advisable for all patients to prescribe vitamin A in drops inside, as well as vitamins Bl, B2, Wb, B12, C, or askorutin.
To prevent dangerous bacterial complications, antibacterial drugs are used (aminopenicillins, second and third generation cephalosporins) in a course of 7-10 days in age dosages.
In the treatment of herpes eczema, immunotropic drugs are also indicated. At present, interferon preparations have proven to be effective in the complex therapy of herpes infections, being the natural factors of nonspecific protection and mediators of immunity, have the broadest spectrum of antiviral action. The most effective and convenient drug in pediatric practice is viferon, recombinant interferon alfa-2b, which has antiviral, anti-proliferative and immunomodulatory activity. The drug is assigned to 2 candles per day, daily for 5 days. Then in a discontinuous course, 1 candle 2 times a day, 3 times a week for 4 weeks, then 2 times a week for 2 months. Infants are prescribed Viferon-1, containing 150000 IU, Viferon-2, containing 500,000 IU, is recommended for children under 7 years old, and Viferon-3, containing 1,000,000 IU, is recommended for children over 7 years old.
External treatment of herpetic eczema is determined by the stage of the process. At the initial stage of the process, bubbles and pustules that are not opened are quenched with a 1% alcohol solution of brilliant green 2-3 times a day. With acute swelling of the face, bright erythema, bleeding erosion, the lesions are treated with 1% aqueous solutions of brilliant green and methylene blue. After extinguishing the lesions with aniline dyes, the rashes are smeared with antiherpetic ointments. Antivirals should be prescribed for external use no later than 48 hours after the onset of a herpetic rash. In the treatment of herpetic eczema in children, 5% acyclovir ointment or cream, 3% vidorabinovy cream, epigenic spray, Viferon ointment, etc. are used externally. On massive hemorrhagic crusts impose 0.5-1% ointment with ethacridine lactate, 2-3% boric naphthalan, or 3% dermatol ointment. Forced removal of hemorrhagic crusts in patients with herpetic eczema is unacceptable, which can lead to severe bleeding, the formation of deep erosions, cracks, and subsequently severe scarring on the face of a child. To accelerate and facilitate the rejection of very dense and massive hemorrhagic crusts on them for 2-4 hours impose a napkin of 4-6 layers of gauze, richly soaked with 5% streptocide liniment, zinc oil, methyluracil ointment or cream with aktovegin and solkoserilom. After the peeling of the crusts, keratoplastic pastes are used (2-3% naphthalan paste, Lassar paste). In case of herpetic eczema, topical use of ointments with corticosteroids is contraindicated.
Topical treatment for lesions of the oral mucosa is also antiviral therapy. In case of herpetic stomatitis, 5% acyclovir ointment, 2% alpisorin ointment, 1% teprofen ointment, and epigenic spray are used in patients with herpetic eczema. These drugs are prescribed 3-4 times a day. Antiviral drugs should be applied to the entire mucous membrane, and not only on the affected areas, as they provide both therapeutic and prophylactic effects. Once a day, the oral cavity is recommended to be treated with a 0.1-0.5% solution of proteolytic enzymes (trypsin, chemotrypsin, pancreatin, etc.), which contribute to the dissolution of necrotic tissue. In the period of extinction of the disease, good results are given by applications of oil solutions of vitamin A, rosehip oil, carotolin, ointment and jelly solcoseryl, ointment with methyluracil.
Regardless of the localization of a skin rash on a child with herpetic eczema, it is necessary to consult an ophthalmologist. In case of herpetic eye disease, antiviral agents are prescribed from the first days: 3% eye ointment of acyclovir 4-5 times a day, interferon in eye drops 6-8 times a day, ophane-IMU, kerecid, semi-dan. The duration of external use of any of the drugs should not exceed 7-10 days. As a means of enhancing the therapeutic effect of antiviral drugs, use antioxidants: 5-10% oil solution of tocopherol in the form of instillation or eye 1% drops of emoxipin 3 times a day. For reparative treatment of the cornea, ophthalmic gel solcoseryl, 3% eye drops of edena are used.
The prognosis of herpetic eczema is always very serious due to the possibility of life-threatening complications. According to the literature, mortality in herpetic eczema ranges from 5-30%. The most common causes of death are sepsis, pneumonia, meningoencephalitis. A significant reduction in the number of complications is observed with timely diagnosis, careful care of children, early and rational treatment in the very first hours after entering the department and establishing the diagnosis.
Herpes Eczema Prevention
In order to prevent herpes eczema, it is necessary to exclude the contact of children suffering from atopic dermatitis or other dermatoses with patients with herpes infection. To this end, patients with herpetic eczema must be hospitalized in an in-cell ward of infectious diseases units for epidemiological indications.