What is Leishmaniasis?
Leishmaniasis – a group of parasitic natural focal, mainly zoonotic, vector-borne diseases, common in tropical and subtropical countries; caused by parasitic protozoa of the genus Leishmania, which are transmitted to humans through mosquito bites.
According to the World Health Organization, leishmaniasis is found in 88 countries of the Old and New Worlds. Of these, 72 are from developing countries, and among these thirteen are the poorest countries in the world. Visceral leishmaniasis occurs in 65 countries.
Leishmaniasis is a neglected disease.
Causes of Leishmaniasis
The causative agents of leishmaniasis are protozoa of the Leishmania genus of the family Trypanosomidae of the class Mastigophora. Currently, there are several dozen types of Leishmania; 17 species exhibit the ability to cause lesions in humans. Leishmania – intracellular parasites that develop in macrophages or cells of the reticuloendothelial system. The life cycle of leishmania proceeds with a change of hosts in the form of two stages – bezgugukovoy (amastigote) in the body of a vertebrate animal or man and flagellar (promastigote) – in the body of arthropod. They reproduce by longitudinal division, morphologically, leishmania are indistinguishable. Dermatotropic types of Leishmania (L. tropica, L. major, L minor, L. aethiopica, etc.) cause skin forms of leishmaniasis. When infected with viscerotropic parasites (L. donovani, L. infantum, L. chagasi, etc.), a systemic, chronic disease occurs. Most types of Leishmania are easy to cultivate in vitro. In cell cultures at 37 ° C, they grow in the form of amastigot, having an oval shape, on cell-free media at 22-27 ° C – in the form of spindle-shaped promasygotes. Leishmania is insensitive to antibiotics, a little more to pentavalent antimony derivatives.
The reservoir and sources of invasion are man and various animals. Among the latter, jackals, foxes, dogs and rodents are most important (gerbils are large, red-tailed, midday, fine-fingered ground squirrel, etc.). The contagion lasts indefinitely for a long time and is equal to the duration of the pathogen in the blood and ulceration of the host’s skin. The duration of cutaneous leishmaniasis in gerbils is usually about 3 months, but can reach 7 months or more.
The transmission mechanism is transmissible, vectors – mosquitoes of the genera Phlebotomus and Lutzomyia. The mosquito P. papatasii, leading in most cases of synanthropic existence, is well studied as a carrier of urban leishmaniasis. The main places of breeding of mosquitoes in the settlements are cellars in residential premises and garbage dumps, in nature there are birds ‘nests, animals’ lairs, rodent holes, caves, rock cracks. In natural foci, the main carriers of Leishmania are P. papatasii, P. caucasicus, P. sergenti. Mosquitoes are active in the twilight and at night. In skin forms of invasion, mosquitoes become infected on leishmaniomas – papules or ulcers in humans, on thickened or ulcerated areas of the ears in gerbils and other animals. In visceral forms of leishmaniasis in humans, parasites are usually not readily available for mosquitoes, so the patient rarely serves as a source of infestation. An exception is the Indian kala-azar, in which Leishmania is often found in the blood and skin lesions, developing in the outcome of the disease. Leishmania gets into the body of a mosquito when sucking the blood of an infected person or animal, in the stomach of which, after a few hours, amastigotes turn into promasigotes. Infectious mosquitoes become 5-8 days after contaminated blood enters the stomach and remain carriers of Leishmania for life. The development of mosquitoes is realized through a complete metamorphosis: egg-larva-pupa-imago. There have been cases of transmission of Leishmania in blood transfusions.
The natural susceptibility of people is high. Immunity is species specific. Strenuous post-infectious immunity is produced only after cutaneous leishmaniasis. Various conditions accompanied by immunodeficiencies significantly reduce parasite resistance.
The main epidemiological signs of leishmaniasis. Indian visceral leishmaniasis (kala-azar), caused by L. donovani, is anthroponosis. It is distributed in a number of districts of Pakistan, Bangladesh, Nepal, China, etc. It is distinguished from time to time by the outbreak of the disease. Mostly teenagers and young people are ill, mainly living in rural areas.
The Mediterranean-Central Asian visceral leishmaniasis, caused by L. infantum, is a zoonosis, the infection reservoir in nature is jackals, foxes, dogs. It is distributed in a number of countries in the Mediterranean, the Near and Middle East, Africa, Kazakhstan, Central Asia and the Transcaucasus. There are natural, semi-synanthropic (rural type) and synanthropic (urban type) centers of invasion. Infection occurs most often in the summer, mostly children from 1 to 5 years of age are ill. In recent years, due to the wide spread of HIV infection, a combination of leishmaniasis and HIV infections, significant changes have occurred in the clinical and epidemiological manifestations of leishmaniasis. Against the background of HIV infection, the concentration of leishmania in the blood and skin of patients is sharply increasing. Such patients, replacing sick dogs, began to play the role of a source of invasion for carriers. The Mediterranean visceral leishmaniasis from a typical zoonosis turned into a transmissible anthroponosis. Maintaining the circulation of the pathogen has become possible in the chain: a sick person — a mosquito — a healthy person. At the same time, as the HIV epidemic developed, further simplification of the development pattern of the epidemic process occurred. The increase in the number of parenteral drug users infected with HIV and leishmania contributed to the formation of direct injection transmission of visceral leishmaniasis. In this case, the utmost simplification of the parasitic system of visceral leishmaniasis has occurred: a sick person is a healthy person. Transfer factors are infected syringes.
South American visceral leishmaniasis (visceral leishmaniasis of the New World), caused by L. chagasi, is close in its manifestations to the Mediterranean-Central Asian leishmaniasis. Mostly sporadic morbidity is noted in a number of countries in Central and South America.
Anthroponotic dermal leishmaniasis of the Old World (Borovsky disease), caused by L. minor, is common in the Mediterranean, the countries of the Near and Middle East, in the western part of the Indian Subcontinent, Central Asia and Transcaucasia. The disease occurs mainly in cities and urban-type settlements inhabited by mosquitoes. Among the local population, children are sick more often, and among visitors – people of all ages. The summer-autumn seasonality is characteristic, which is connected with the activity of carriers.
Zoonotic dermal leishmaniasis of the Old World (Pendin ulcer) is caused by L. major. The main reservoir of the invasion is rodents (large and red gerbil, etc.). Distributed in the countries of the Middle East, North and West Africa, Asia, Turkmenistan and Uzbekistan. Endemic foci are found mainly in the desert and semi-desert, in the countryside and on the outskirts of cities. Summer seasonality of infections is determined by the period of activity of mosquitoes. Mostly children are ill, outbreaks of diseases among people of different ages are possible.
Zoonotic cutaneous leishmaniasis of the New World (Mexican, Brazilian and Peruvian cutaneous leishmaniasis) caused by L. mexicana, L. braziliensis, L. peruviana, L. uta, L. amazoniensis, L. pifanoi, L. venezuelensis, L. garnhami, L. panamensis, registered in Central and South America, as well as in the southern regions of the United States. The natural reservoir of pathogens – rodents, numerous wild and domestic animals. Diseases are found in rural areas, mainly in the rainy season. People of all ages get sick. Typically, the infection occurs at the time of work in the forest, hunting, etc.
Pathogenesis during Leishmaniasis
When the leishmania mosquito bites in the form of promastigotes penetrate into the human body. Their primary reproduction in macrophages is accompanied by the transformation of pathogens into amastigote (bezggutikova form). At the same time, productive inflammation develops, and a specific granuloma forms at the site of introduction. It consists of macrophages containing pathogens, reticular, epithelioid and giant cells. Formed a primary affect in the form of papules; later, in visceral leishmaniasis, it resolves without a trace or is scarring.
In cutaneous leishmaniasis, destruction of the skin at the site of the former tubercle, ulceration and then healing of the ulcer with the formation of a scar develop. Spreading lymphogenous way to the regional lymph nodes, Leishmania provoke the development of lymphangitis and lymphadenitis, the formation of limited skin lesions in the form of consecutive Leishmania. The development of tuberculoid or diffuse infiltrating cutaneous leishmaniasis is largely due to the state of reactivity of the organism (hyperergy or hypoergy, respectively).
Along with the skin forms of the disease, one can observe the so-called skin-mucous forms with ulceration of the mucous membranes of the nasopharynx, larynx, trachea and the subsequent formation of polyps or deep destruction of soft tissues and cartilage. These forms are registered in the countries of South America.
In visceral leishmaniasis, primary affect is less common, mainly in children. From the site of inoculation, the pathogens disseminate to the lymph nodes, then to the liver, spleen, bone marrow, intestinal wall, sometimes to the kidneys, adrenal glands and lungs, where they enter the CMF cells and multiply in them. This causes functional and morphological disorders in the organs of the reticulohistiocytic system (systemic parasitic reticulohistiocytosis). The development of delayed-type hypersensitivity contributes to the destruction of Leishmania; in such cases, the disease proceeds in a subclinical or latent form. Against the background of reduced reactivity or immunosuppression, Leishmania actively proliferate, causing fever and other manifestations of intoxication, which is caused by the products of parasite metabolism, the development of pathological changes in the internal organs and their dysfunction due to generalized endotheliosis. In the liver, hypertrophy of stellate endotheliocytes (Kupffer cells) leads to compression and atrophy of hepatocytes, the development of interlobular fibrosis. Atrophy of the pulp of the spleen (sometimes with necrosis and heart attacks) and germinal centers of the lymph nodes develops. Violations of bone marrow hemorrhage lead to anemia. Cachexia develops.
The resulting antibodies exhibit mild protective activity, since most leishmania are parasitic intracellularly or localized in granulomas. At the same time, high titers of auto-antibodies are formed, which indicates the development of immunopathological processes. Against this background, there are secondary infections, the formation of kidney amyloidosis, hypochromic anemia.
Convalescents develop a stable homologous immunity.
Symptoms of Leishmaniasis
In accordance with the characteristics of the clinic, etiology and epidemiology of leishmaniasis are divided into the following types.
Visceral leishmaniasis (kala azar)
- Zoonotic: Mediterranean-Central Asian (children’s kala-azar), East African (dum-dum fever), skin and mucous leishmaniasis (leishmaniasis of the New World, nasopharyngeal leishmaniasis).
- Anthroponotic (Indian kala azar).
Cutaneous leishmaniasis
- Zoonotic (rural type of Borovsky disease, pendinsky ulcer).
- Anthroponotic (urban type Borovskiy disease, Ashgabat ulcer, Baghdad furuncle).
- Skin and skin-mucous leishmaniasis of the New World (Espundiya, Breda’s disease).
- Ethiopian cutaneous leishmaniasis.
Visceral Mediterranean-Asian Leishmaniasis.
Incubation period. Varies from 20 days to 3-5 months, in rare cases up to 1 year or more. In young children and rarely in adults, long before the general manifestations of the disease, a primary affect in the form of a papule occurs.
The initial period of the disease. Characterized by the gradual development of weakness, loss of appetite, weakness, pallor of the skin, a slight increase in the spleen. Slightly increased body temperature.
The period of height. It usually begins with a rise in body temperature to 39-40 ° C. Fever takes on a wave-like or irregular nature and lasts from several days to several months with a change in episodes of high temperature and remission. In some cases, the body temperature during the first 2-3 months is subfebrile or even normal.
On examination of patients, polylimphadenopathy (peripheral, peribronchial, mesenteric, and other lymph nodes), enlargement and thickening of the liver, and even more of the spleen, painless on palpation, are determined. In cases of bronchoadenitis, cough is possible, pneumonia of a secondary bacterial nature is common.
As the disease progresses, the condition of the patients progressively worsens. Weight loss (up to cachexia) and hypersplenism develop. Bone marrow lesions lead to progressive anemia, granulocytopenia and agranulocytosis, sometimes with necrosis of the mucous membranes of the oral cavity. Often there are manifestations of hemorrhagic syndrome: hemorrhages in the skin and mucous membranes, bleeding from the nose, gastrointestinal tract. Fibrous changes in the liver lead to portal hypertension with edema and ascites, aided by progressive hypoalbuminemia.
Due to hypersplenism and high standing of the diaphragm, the heart shifts somewhat to the right, its tones become deaf, tachycardia and arterial hypotension develop. These changes, along with anemia and intoxication, lead to the appearance and increase of signs of heart failure. Possible diarrhea, menstrual disorders, impotence.
The terminal period. They observe cachexia, a drop in muscle tone, thinning of the skin, the development of protein-free edema, severe anemia.
The disease can manifest itself in acute, subacute and chronic forms.
- Acute form. Occasionally met in young children. It develops rapidly, without treatment, it quickly ends in a lethal outcome
- Subacute form. Meet more often. Severe clinical manifestations lasting 5-6 months are characteristic.
- Chronic form. It develops most often, often proceeds subclinically and latently.
With visceral anthroponotic leishmaniasis (Indian Kala-azar) in 10% of patients after a few months (up to 1 year), so-called leishmanoids appear on the skin after therapeutic remission. They are small nodules, papillomas, erythematous spots or patches of skin with reduced pigmentation, which contain Leishmania for a long time (years and decades).
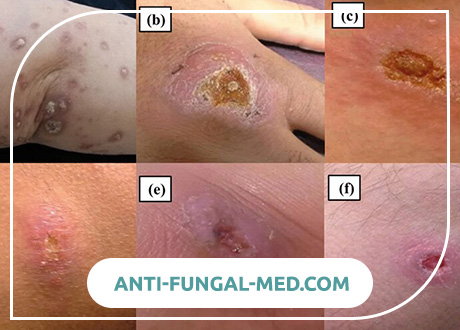
Skin zoonotic leishmaniasis (pendinsky ulcer, Borovsky disease). Meet in tropical and subtropical countries. The incubation period varies from 1 week to 1.5 months, an average of 10-20 days. In the place of the entrance gate, a primary leishmanioma appears, initially representing a smooth pink-colored papule with a diameter of 2-3 mm. The size of the tubercle is rapidly increasing, while it sometimes resembles a furuncle, but painless or slightly painful on palpation. After 1-2 weeks, necrosis begins in the center of the leishmanioma, resembling an abscess head, and then a painful ulcer is formed up to 1-1.5 cm in diameter, with undermined edges, a powerful rim of infiltration and copious serous purulent or sukrovichny exudate; Small secondary hillocks, the so-called “seedlings,” which also ulcerate and form ulcerative fields when merged, often form around it. So a consistent leishmanioma is formed. Leishmanias are more often localized in open parts of the body, their number varies from a few to dozens. The formation of ulcers in many cases accompanies the development of painless lymphangitis and lymphadenitis. After 2-6 months, epithelization of the ulcers and their scarring begin. The total duration of the disease does not exceed 6-7 months.
Diffuse infiltrating leishmaniasis. It is characterized by severe infiltration and thickening of the skin with a large area of distribution. Gradually infiltrate resolves without a trace. Minor ulcerations are observed only in exceptional cases; they heal with scar formation. This variant of cutaneous leishmaniasis is very rare in older people.
Tuberculoid cutaneous leishmaniasis. Sometimes observed in children and young people. It is distinguished by the formation of small bumps around the scars or on them. The latter can grow and merge with each other. In the dynamics of the disease, they occasionally ulcerate; later ulcers heal with scarring.
Cutaneous anthroponotic leishmaniasis. It has a long incubation period of several months or even years and two main features: slow development and less pronounced skin lesions.
Complications and prognosis
Launched leishmaniasis can complicate pneumonia, purulent necrotic processes, nephritis, agranulocytosis, hemorrhagic diathesis. The prognosis of severe and complicated forms of visceral leishmaniasis with late treatment is often unfavorable. In light forms, spontaneous recovery is possible. In cases of cutaneous leishmaniasis, the prognosis for life is favorable, but cosmetic defects are possible.
Diagnosis of Leishmaniasis
Visceral leishmaniasis should be distinguished from malaria, typhoid-paratyphoid diseases, brucellosis, lymphogranulomatosis, leukemia, sepsis. At establishment of the diagnosis, data of the epidemiological anamnesis are used, testifying to the patient’s stay in the endemic foci of the disease. When examining a patient, it is necessary to pay attention to prolonged fever, polylimfadenopatigo, anemia, weight loss, hepatolienal syndrome with a significant increase in the spleen.
Manifestations of cutaneous zoonotic leishmaniasis differentiate from similar local changes in leprosy, skin tuberculosis, syphilis, tropical ulcers, epithelioma. It is necessary to take into account the phasic formation of leishmaniomas (painless papule – necrotic changes – an ulcer with saped edges, a rim of infiltration and a serous-purulent exudate – scar formation).
Laboratory diagnosis of leishmaniasis
In the hemogram, signs of hypochromic anemia, leukopenia, neutropenia and relative lymphocytosis, aneosinophilia, thrombocytopenia, and a significant increase in ESR are determined. Poikilocytosis, anisocytosis, anisochromia are characteristic, agranulocytosis is possible. Hypergammaglobulinemia is noted.
In cutaneous leishmaniasis, pathogens can be found in material obtained from tubercles or ulcers; in visceral, in smears and thick drops of blood stained by Romanovsky-Giemsa, more often (95% of positive results) in smears of bone marrow. The culture of the pathogen (promasigote) can be obtained by sowing punctate on Wednesday NNN. Sometimes a lymph node or even liver and spleen are biopsied to detect leishmania. Serological reactions are widely used – RSK, ELISA, RFP, RLA, etc., biological tests on hamsters or white mice. During the recovery period, the skin test with leishmanin (Montenegro reaction), which is used only in epidemiological studies, becomes positive.
Leishmaniasis Treatment
In visceral leishmaniasis, pentavalent antimony preparations are used (solusurmin, neostybozane, glucantim, etc.) in the form of daily intravenous fluids in increasing doses starting from 0.05 g / kg. The course of treatment is 7-10 days. With insufficient clinical efficacy of drugs prescribed amphotericin B 0.25-1 mg / kg slowly intravenously in 5% glucose solution; the drug is administered every other day up to 8 weeks. Pathogenetic therapy and prevention of bacterial complications are carried out according to well-known schemes.
In cases of cutaneous leishmaniasis, at the early stage of the disease, the hillocks are punctured by solutions of mepacrine, monomitsin, hexamine, berberine sulfate; apply ointments and lotions using these tools. When ulcers are formed, intramuscular injections of monomitsin are prescribed in 250 thousand U units (for children 4-5 thousand U / kg) 3 times a day, the course dose of the drug is 10 million U. You can carry out treatment with aminoquinol (0.2 g 3 times a day, for the course – 11-12 g of the drug). Apply laser irradiation of ulcers. Pentavalent antimony and amphotericin B are prescribed only in severe cases of the disease.
Drugs of choice: antimonyl gluconate sodium at 20 mg / kg i.v. or v / m once a day with a course for 20-30 days; meglumine antimoniat (glucantim) 20-60 mg / kg deep i / m once a day with a course for 20-30 days. When the disease recurs or the treatment is not sufficiently effective, a repeated course of injections should be given within 40-60 days. Effectively the additional appointment of allopurinol 20-30 mg / kg / day in 3 doses inside.
Alternative drugs for the recurrence of the disease and pathogen resistance: amphotericin B 0.5-1.0 mg / kg IV per day or pentamidine IM / 3-4 mg / kg 3 times a week for 5-25 weeks. In the absence of the effect of chemotherapy, human recombinant y-interferon is further prescribed.
Surgery. According to the testimony of conducting splenectomy.
Prevention of Leishmaniasis
The fight against animal carriers of Leishmania is carried out in an organized and on a large scale only in case of zoonotic dermal and visceral leishmaniasis. Carry out deratization activities, improvement of populated areas, the elimination of wastelands and landfills in them, drainage of the basements, treatment of residential, courtyard and livestock buildings with insecticides. Recommended the use of repellents, mechanical means of protection against mosquito bites.
After the identification and treatment of sick people, they neutralize the source of the invasion. In small groups, chemoprophylaxis is prescribed with chloridine (pyrimethamine) administration during the epidemic season. Immunoprophylaxis of zoonotic cutaneous leishmaniasis is carried out by a live culture of promasigotes of the virulent L. major strain in the interepidemic period among people traveling to endemic foci or non-immune individuals living in these foci.