What is Tularemia?
Tularemia is an acute infectious natural focal disease with damage to the lymph nodes, skin, sometimes the eyes, throat and lungs and accompanied by severe intoxication.
Brief History
In 1910, near the Lake Tulare in California, D. McCoy discovered a gopher disease in gophers, reminiscent of the clinical picture of bubonic plague. Soon, he and Ch. Chapin isolated the pathogen from sick animals, which was named Bacterium tularense (1912). Later it was found out that people are susceptible to this infection, and on the proposal of E. Francis (1921) it was called tularemia. Later, the pathogen was named after Francis, who studied it in detail.
Causes of Tularemia
The causative agent is immobile gram-negative aerobic encapsulated bacteria F. tularensis of the genus Francisella of the family Brucellaceae. Show pronounced polymorphism; most often have the form of small coccobacilli.
In bacteria, three subspecies are distinguished:
- non-arctic (African);
- Central Asian;
- Holarctic (Euro-Asian).
The latter includes three biological variants: Japanese biovar, erythromycin-sensitive and erythromycin-resistant. The intraspecific differentiation of the causative agent of tularemia is based on the differences of subspecies and biovars in a number of phenotypic characters: biochemical activity, the composition of higher fatty acids, the degree of pathogenicity for humans and animals, sensitivity to certain antibiotics, as well as environmental characteristics and the range of the pathogen. O and Vi antigens were found in bacteria. Bacteria grow on vitelline or agar media supplemented with rabbit blood or other nutrients. From laboratory animals, white mice and guinea pigs are sensitive to infection. Outside the host organism, the pathogen persists for a long time. So, in water at 4 ° C it remains viable for 1 month, on straw and grain at temperatures below 0 ° C – up to 6 months, at 20-30 ° C – up to 20 days, in the skins of animals that fell from tularemia, at 8 -12 “C – more than 1 month. Bacteria are unstable to high temperature and disinfectants. For disinfection use a 5% phenol solution, a mercuric chloride solution 1: 1000 (kills bacteria within 2-5 minutes), 1-2% formalin solution (destroys bacteria for 2 hours), 70 ° ethanol, etc. For complete disinfection of the bodies of infected animals, they should be kept for at least 1 day in a disinfectant solution, then autoclave and burn.
Epidemiology
The reservoir and source of infection are numerous species of wild rodents, hare, birds, dogs, etc. Bacteria are isolated from 82 species of wild, as well as from domestic animals (sheep, dogs, artiodactyls). The main role in maintaining the infection in nature belongs to rodents (water rat, common vole, muskrat, etc.). A sick person is not dangerous to others.
The transmission mechanism is multiple, most often transmissible. The causative agent is preserved in nature in the cycle “tick – animal”, transmitted to agricultural animals and birds by ticks and blood-sucking insects. Specific carriers of tularemia are ixodid ticks. A person becomes infected with tularemia as a result of direct contact with animals (skinning, collection of dead rodents, etc.), as well as by alimentary route through food infected with rodents and water. Often infection occurs through blood-sucking vectors (ticks, mosquitoes, fleas, horseflies and other arthropods). Possible infection by the respiratory route (by inhaling infected dust from grain, straw, vegetables). Cases of human diseases were recorded in industries associated with the processing of natural raw materials (sugar, starch and syrup, distilleries, hemp plants, elevators, etc.), in meat processing plants, when slaughtering sheep and cattle, which had infected ticks, outskirts of cities located near natural foci. There are known cases of the introduction of infection during the transportation of products and raw materials from areas unfavorable for tularemia.
The natural susceptibility of people is high (almost 100%).
The main epidemiological signs. Tularemia is a common natural focal disease that occurs mainly in landscapes of the temperate climatic zone of the Northern Hemisphere. The wide spread of the pathogen in nature, the involvement of a large number of warm-blooded animals and arthropods in its circulation, the seeding of various environmental objects (water, food) also determine the characteristics of the epidemic process. There are various types of foci (forest, steppe, meadow-field, bog, in the river valley, etc.). Each type of foci has its own species of animals and blood-sucking arthropods involved in the transmission of the pathogen. Among patients, adults predominate; often the incidence is associated with the profession (hunters, fishermen, agricultural workers, etc.). Men get sick 2-3 times more often than women. Anthropurgic foci of tularemia occur when infected rodents migrate from their habitats to settlements where they come into contact with synanthropic rodents. Tularemia remains a disease of the countryside, however, a steady increase in the incidence of urban population is currently noted. Tularemia is recorded throughout the year, but more than 80% of cases occur in summer and autumn. In recent years, the incidence is sporadic. In some years, local transmissible, commercial, agricultural, and aquatic outbreaks are noted, less frequently other types of outbreaks. Transmissible outbreaks are caused by transmission of the pathogen by blood-sucking dipterans and occur in the foci of tularemia epizootics among rodents. Transmissive outbreaks usually begin in July or June, peak in August and cease in September-October; haymaking and harvesting contribute to an increase in the incidence.
The industrial type of outbreak is usually associated with the capture of a water rat and muskrat. Commercial outbreaks occur in spring or early summer during the flood season, and their duration depends on the harvesting period. Infection occurs by contact with animals or skins; the pathogen penetrates through lesions on the skin, in connection with which axillary buboes more often occur, often without ulcers at the site of insertion.
Water outbreaks determines the entry of pathogens into open waters. The main pollutant of water are water voles that live along the coast. Diseases usually occur in the summer with a rise in July. Diseases associated with field work and the use of drinking water from random reservoirs, wells, etc. In 1989-1999. the proportion of isolates of the causative agent of tularemia from water samples reached 46% or more, which indicates the important epidemiological significance of reservoirs as long-term reservoirs of infection.
Agricultural outbreaks occur when airborne aerosol is inhaled when working with straw, hay, grain, feed, and urine contaminated with sick rodents. Pulmonary, rarely abdominal and angina-bubonic forms predominate. The household type of outbreaks characterizes infection in the home (at home, on the estate). Infection is also possible during sweeping, bulkheading and drying of agricultural products, distributing pet food, and eating contaminated foods.
Pathogenesis during Tularemia
Bacteria enter the human body through the skin (even intact), mucous membranes of the eyes, respiratory tract and gastrointestinal tract. In the area of the entrance gate, the localization of which largely determines the clinical form of the disease, the primary affect often develops in the form of successively replacing spots, papules, vesicles, pustules and ulcers. Subsequently, tularemia sticks enter the regional lymph nodes, where they multiply and develop an inflammatory process with the formation of the so-called primary bubo (inflamed lymph node). With the death of francisella, a lipopolysaccharide complex (endotoxin) is released, which enhances the local inflammatory process and, when it enters the blood, causes the development of intoxication. Bacteremia with disease does not always occur. In the case of hematogenous dissemination, generalized forms of infection develop with toxic-allergic reactions, the appearance of secondary buboes, and damage to various organs and systems (primarily the lungs, liver and spleen). In the lymph nodes and affected internal organs, specific granulomas are formed with central areas of necrosis, an accumulation of granulocytes, epithelial and lymphoid elements. The formation of granulomas is facilitated by incomplete phagocytosis due to the properties of the pathogen (the presence of factors that prevent intracellular killing). The formation of granulomas in primary buboes often leads to their suppuration and spontaneous dissection, followed by prolonged healing of the ulcer. Secondary buboes usually do not suppurate. In the case of replacement of necrotic areas in the lymph nodes with connective tissue, suppuration does not occur, buboes are absorbed or sclerosed.
Tularemia Symptoms
In accordance with the clinical classification, the following forms of tularemia are distinguished:
- by localization of the local process: bubonic, ulcerative-bubonic, ocular-bubonic, anginal-bubonic, pulmonary, abdominal, generalized;
- by the duration of the course: acute, protracted, recurrent;
- by severity: mild, moderate, severe.
Incubation period. It lasts from 1 to 30 days, most often it is 3-7 days.
Symptoms of the disease, common to all clinical forms, are expressed in an increase in body temperature to 38-40 ° C with the development of other symptoms of intoxication – chills, headache, muscle pain, general weakness, anorexia. Fever can be remitting (most often), constant, intermittent, wavy (in the form of two or three waves). The duration of the fever is different, from 1 week to 2-3 months, most often it lasts 2-3 weeks. When examining patients, hyperemia and pastiness of the face, as well as the mucous membrane of the mouth and nasopharynx, injection of the sclera, and conjunctival hyperemia are noted. In some cases, exanthema of a different nature appears: erythematous, maculopapular, roseolous, vesicular or petechial. The pulse is reduced (relative bradycardia), blood pressure is lowered. A few days after the onset of the disease, hepatolienal syndrome develops.
The development of various clinical forms of the disease is associated with the mechanism of infection and the entrance gate of the infection, which determine the localization of the local process. After penetration of the pathogen through the skin, a bubonic form develops in the form of a regional lymphadenitis infection (bubo) with respect to the gate. Perhaps isolated or combined damage to various groups of lymph nodes – axillary, inguinal, femoral. In addition, secondary buboes can form with hematogenous dissemination of pathogens. There is soreness, and then an increase in lymph nodes to the size of a hazelnut or a small chicken egg. In this case, pain reactions gradually decrease and disappear. The contours of the bubo remain distinct, the phenomena of periadenitis are insignificant. In the dynamics of the disease, buboes slowly (sometimes over several months) dissolve, fester with the formation of a fistula and discharge of creamy pus, or become sclerosed.
Forms of the disease
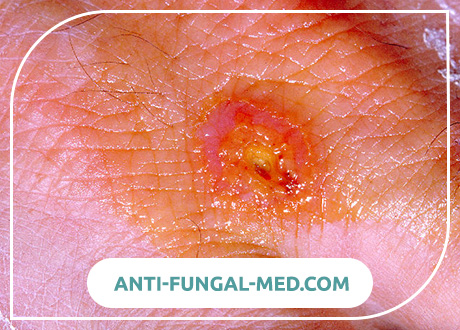
Ulcerative bubonic form. It develops more often with transmissible infection. At the site of introduction of the microorganism, a spot, papule, vesicle, pustule, and then a shallow ulcer with raised edges successively replace each other for several days. The bottom of the ulcer is covered with a dark crust in the form of a “cockade”. At the same time, regional lymphadenitis (bubo) develops. Subsequently, scarring of the ulcer occurs slowly.
In cases of penetration of the pathogen through the conjunctiva, an ocular-bubonic form of tularemia occurs. In this case, damage to the mucous membranes of the eyes occurs in the form of conjunctivitis, papular, and then erosive and ulcerative formations with the separation of yellowish pus. Corneal lesions are rare. These clinical manifestations are accompanied by pronounced edema of the eyelids and regional lymphadenitis. The course of the disease is usually quite severe and prolonged.
Angina-bubonic form. It develops after the penetration of the pathogen with infected food or water. Patients complain of moderate sore throat, difficulty swallowing. On examination, the tonsils are hyperemic, enlarged and edematous, adhered to the surrounding tissue. On their surface, more often on one side, grayish-white necrotic plaques are formed, which can be removed with difficulty. Expressed edema of the palatine arches and uvula. Subsequently, the destruction of the amygdala tissue occurs with the formation of deep, slowly healing ulcers, followed by the formation of a scar. Tularemia buboes occur in the submandibular, cervical and parotid regions, more often on the side of the affected amygdala.
Abdominal form. It develops as a result of damage to the mesenteric lymph nodes. Clinically manifested by severe abdominal pain, nausea, occasionally vomiting, anorexia. Diarrhea sometimes develops. On palpation, soreness near the navel is noted, positive symptoms of peritoneal irritation are possible. As a rule, hepatolienal syndrome is formed. It is rarely possible to palpate the mesenteric lymph nodes; their enlargement is established using ultrasound.
Pulmonary form. It proceeds in the form of a bronchitic or pneumonic variant.
- The bronchitic variant is due to the defeat of the bronchial, mediastinal, paratracheal lymph nodes. Against the background of moderate intoxication, a dry cough appears, pain behind the sternum, dry wheezing is heard in the lungs. Usually this option is easy and ends with recovery in 10-12 days.
- The pneumonic variant is characterized by an acute onset, a sluggish, debilitating course with a high, prolonged fever. Pathology in the lungs is clinically manifested by focal pneumonia. Pneumonia is characterized by a rather severe and acyclic course, a tendency to develop complications (segmental, lobular or disseminated pneumonia, accompanied by an increase in the above groups of lymph nodes, bronchiectasis, abscesses, pleurisy, cavities, gangrene of the lungs).
Generalized form. Clinically similar to typhoid-paratyphoid infections or severe sepsis. High fever becomes abnormally remitting and persists for a long time. Symptoms of intoxication are expressed: headache, chills, myalgia, weakness. Confusion of consciousness, delirium, hallucinations are possible. The pulse is labile, the heart sounds are muffled, and the blood pressure is low. In most cases, from the first days of the disease, hepatolienal syndrome develops. In the future, the appearance of persistent exanthema of a roseolous and petechial nature with localization of elements of the rash on symmetrical parts of the body – forearms and hands, legs and feet, on the neck and face is possible. With this form, the development of secondary buboes is possible, caused by hematogenous dissemination of pathogens, and metastatic specific pneumonia.
Complications
In most cases, they develop in a generalized form. The most common are secondary tularemia pneumonia. Infectious toxic shock is possible. In rare cases, meningitis and meningoencephalitis, myocarditis, polyarthritis, etc. are observed.